Phage therapy: from a renaissance to a therapeutic revolution
Phage therapy: from a renaissance to a therapeutic revolution
Initially described as the "rebirth of an old treatment," phage therapy is now undergoing a true revolution. Driven by the urgency of antibiotic resistance, this century-old approach is now part of the modern therapeutic arsenal.
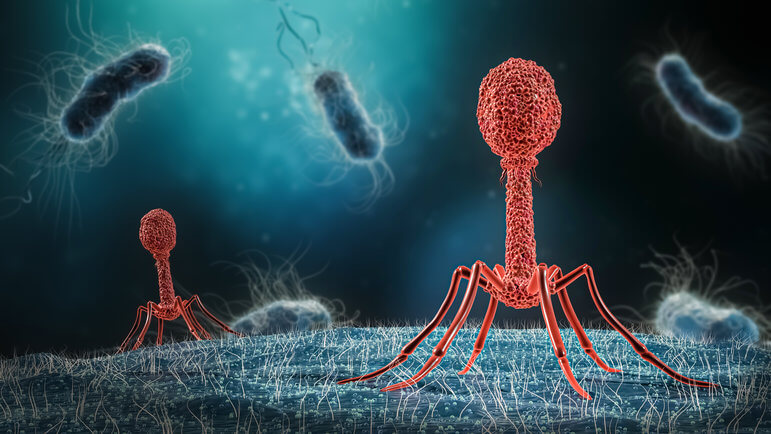
Phages specifically target a bacterium, replicate within it, and lyse it to spread. Royalty-free / iStock / Getty Images Plus / via Getty Images
Phage therapy relies on the use of bacteriophages, natural viruses that specifically target a bacterium, within which they replicate to spread. Their specificity protects commensal bacteria, and their ability to self-magnify at the injection site gives them unique pharmacokinetic characteristics.
In France, phage therapy has seen significant growth over the past five years, thanks to the development of pharmaceutical-grade phages. These can be used on a compassionate basis in clinical situations where life or function is at risk (complex and/or recurrent osteoarticular, pulmonary, or endovascular infections) or during clinical trials. The implementation of multidisciplinary consultation meetings within the "PHAGEinLYON Clinic" program now allows for the collaborative validation of indications and various treatment regimens, based on the clinical presentation.
Access to more pharmaceutical-grade phages targeting a wider range of pathogenic bacteria, and the use of artificial intelligence to optimize and personalize phage selection, are under investigation. Regulatory innovations are also expected to harmonize quality, manufacturing, and testing standards for phages in order to ensure their safe therapeutic use across Europe.
Phage therapy, developed by Félix d'Hérelle in the 1920s, has had a paradoxical history. After generating considerable enthusiasm, it gradually faded into obscurity with the rise of antibiotics, which offered a broader spectrum of action and were easier to use. Today, faced with the alarming increase in antibiotic resistance, this century-old therapy is emerging as a therapeutic alternative. Tristan Ferry, professor of infectious diseases and coordinator of the Reference Center for Complex Osteoarticular Infections (Crioac) at the Hospices Civils de Lyon (HCL), accredited by the Ministry of Health, offers us an overview of the major advances that are reshaping the landscape of the fight against resistant bacterial infections.
What is phage therapy?
Professor Tristan Ferry.
They are characterized by their specificity for a given bacterial species or subspecies, which they recognize primarily by the presence of specific components of the bacterial cell wall, often polysaccharides. Using tail fibers, they attach to the cell wall before penetrating the bacterium, where they replicate. The synthesis of specialized enzymes, depolymerases, capable of degrading the bacterial biofilm, or, more frequently, endolysins, causing bacterial lysis, allows the release of new virions capable of infecting new bacteria.
The principle is to generate a viral infection, not in the patient, but within the bacteria that infect the patient, in order to act on bacterial replication, and on the bacterial biofilm if one had formed.
What are the advantages compared to conventional antibiotics?
The greatest advantage of phage therapy is its specificity of action. By precisely targeting the pathogenic bacteria, the integrity of the intestinal microbiota or other commensal flora is preserved.
Another major theoretical advantage is the phenomenon of self-amplification. Unlike antibiotics, whose plasma concentration gradually decreases after administration, phages can, in theory, multiply at the very site of infection. This unique characteristic gives phage therapy a distinctive pharmacokinetic profile, potentially advantageous in certain infectious contexts.
Finally, the ability of phages to degrade bacterial biofilm opens up promising therapeutic perspectives, particularly for the hope of preserving valuable implants, and thus avoiding many surgeries with a risk of complications.
And the limits ?
Just as with antibiotics, resistance phenomena are observed in nature. This "
Furthermore, the pharmacokinetic fate of phages remains uncertain. Administration of natural viruses can induce an immune response in the patient, leading to the production of neutralizing antibodies against these viruses, thus compromising efficacy. Current knowledge does not yet allow us to determine whether these antibodies pre-exist or whether their development depends on the administration method, thereby creating interindividual variability in treatment response. Even when clinical situations are identified as potentially suitable, the optimal administration methods (route, dose, frequency) remain to be defined to maximize the effect.
Although several trials are underway, both to explore therapeutic potential and to study technical feasibility, they are encountering significant methodological difficulties. Indeed, traditional methodologies for evaluating antibiotics are not fully applicable to phage therapy trials. Double-blind, phase 3 clinical trials, the gold standard for therapeutic evaluation, are difficult to conduct, especially given that this is a personalized therapy.
In which therapeutic areas is phage therapy currently used?
In France, phage therapy is used on a compassionate basis, an exceptional measure which allows access to drugs that do not have marketing authorization and without which no therapeutic option is available, provided that the efficacy-safety ratio is presumed favorable in view of the available data.
Issued by the National Agency for the Safety of Medicines and Health Products (ANSM), it is reserved for patients whose vital or functional prognosis is at risk and who benefit from multidisciplinary care in referral centers.
This administrative procedure, specifically French, allows early access to pharmaceutical-grade phages (the standard being the "
The main indications, which must be validated collectively in a multidisciplinary tumor board meeting, concern complex osteoarticular infections, particularly prosthetic joint infections, but also recurrent chronic pulmonary infections, such as repeated exacerbations in patients with chronic lung disease with respiratory function impairment and/or acquisition of multidrug resistance. It can also be considered for refractory endovascular infections, such as infective endocarditis or recurrent bacteremia.
What is the current status in France regarding its use in clinical practice?
Approximately 150 patients have been treated with phage therapy in France over the past five years. Among them, 120 to 130 benefited from the expertise of the "
The RCPs
This personalized approach encompasses the entire care pathway, from surgery and interventional radiology procedures to antibiotic therapy and the pharmaceutical preparation of bacteriophages proven effective against the patient's bacterial strain. Phage therapy is a rapidly developing, personalized, and precision-based adjunctive therapy to traditional care.
How exactly does the care of a candidate patient unfold?
The physician can complete the process online, on the HCL's secure institutional portal, where a form is available. They fill in the patient-candidate's information. The application, thus formalized, is discussed in a multidisciplinary team meeting (RCP) within the framework of the "
This method is part of an innovative ecosystem. Supported by the Hospices Civils de Lyon Foundation, the platform connects medical teams with producers of pharmaceutical-grade phages, whether private or military, French or foreign. Depending on the bacterium involved, it is then possible to verify the availability of phages that could be offered to the patients concerned, and subsequently determine their ability to infect the patient's bacteria.
When one or more phages are found to be active, the case is discussed again in a multidisciplinary team meeting (MDT) to define the therapeutic strategy and propose a personalized administration regimen adapted to the clinical situation. For example, for a pulmonary infection, aerosol administration will be preferred, except in the case of a lung abscess where bronchoscopy (possibly combined with intravenous administration) will be used as an adjunct. In the case of osteoarticular infections, local administration is preferred, possibly supplemented by intravenous administration. The duration of treatment is generally between 7 and 10 months.
All these proposals are shared with the ANSM, and the active phages are then ordered, sometimes imported, and then prepared by the hospital pharmacist, and this
Follow-up is exclusively in-hospital. Some adverse effects may occur. Since the bacteriophages used are considered harmless to humans, these effects are primarily attributable to bacterial residues that may remain in the preparations. These residues are potentially pyrogenic or may induce bronchospasm when administered via inhalation. Furthermore, an adaptive immune response with the production of neutralizing antibodies may compromise therapeutic efficacy and could potentially generate cross-reactions.
What are the major innovations expected in this field?
Artificial intelligence could play a major role in the very short term, particularly in predicting the lytic effectiveness of phages on the patient's bacterial strain.
Phage therapy is inherently highly personalized. This specificity, sometimes restricted to certain bacterial serotypes or subspecies, requires manufacturers to establish extensive phage banks. For example, to cover 90
The European Medicines Agency (EMA) published a directive on October 16, 2025, concerning the qualitative aspects of phage therapy. This document aims to establish a harmonized framework for the quality, manufacturing, and control requirements of phage products. Between medicines subject to Good Manufacturing Practices (GMP) and compounded preparations made in hospitals, governed by Good Preparation Practices, regulatory bodies are proceeding cautiously, as the issue is complex when dealing with viruses, but significant progress is being made ( see Box ) .
In France, therapeutic bacteriophages fall under the status of biological medicines and their quality complies with Good Manufacturing Practices ( GMP). Their prescription is subject to a specific exemption framework in the absence of a marketing authorization. Compounded preparations made in hospital pharmacies from phage suspensions or lyophilized products follow good preparation practices. |
In conclusion ?
Phage therapy represents a promising approach for treating severe bacterial infections, including those involving implants or antibiotic-resistant bacteria. Its development in France, particularly thanks to
Based on an interview with Tristan Ferry, professor of infectious diseases and coordinator of the reference center for complex osteoarticular infections (Crioac) of the Hospices civils de Lyon (HCL).
Article written by : Anne-Solène Naudon, article taken from, copyright belongs to : https://www.vidal.fr/actualites/37232-la-phagotherapie-d-une-renaissance-a-une-revolution-therapeutique.html
.png)

.png)
Comments
Post a Comment